VA Rating for Neck Pain: What Veterans Should Know
Neck pain is one of the most commonly underrated musculoskeletal conditions in the VA disability system. The VA evaluates cervical spine disabilities using strict mechanical criteria—meaning a rating is determined primarily by measurable angles, documented range of motion, and objective functional loss rather than the subjective severity of daily pain. The VA evaluates cervical, spine disabilities using specific range of motion and functional loss criteria, which means the medical record and examination findings play an important role in how the condition is evaluated.
This guide breaks down the regulatory framework governing a VA rating for neck pain, explains the specific metrics the VA uses to assign percentages, and identifies the medical evidence and documentation that help provide a complete clinical picture for evaluation.
TL;DR
- Diagnosis is the entry point: The claim typically requires a diagnosis of Cervical Strain (DC 5237) or Degenerative Arthritis (DC 5003) before evaluation can proceed
- Range of motion drives the rating: The percentage assigned is determined primarily by measurable degrees of forward flexion, not subjective pain levels
- The 30% threshold: A 30% rating requires forward flexion of the cervical spine of 15 degrees or less
- Painful motion protects against 0%: Under 38 CFR 4.59, pain during motion—even with preserved range of motion—requires a minimum compensable rating
- Examination accuracy is critical: If a goniometer is not used to measure joint angles during the C&P exam, the results may be inaccurate and subject to challenge
- Secondary claims add value: Cervical radiculopathy and cervicogenic migraines are rated separately from the neck condition and represent additional compensation potential

How the VA Defines Cervical Spine Disability
Before addressing rating percentages, it is necessary to understand how the VA classifies neck disability. The VA does not rate “neck pain” in isolation—it rates the underlying diagnosed condition causing that pain. The specific medical diagnosis determines which Diagnostic Code applies and which evidentiary criteria govern the evaluation.
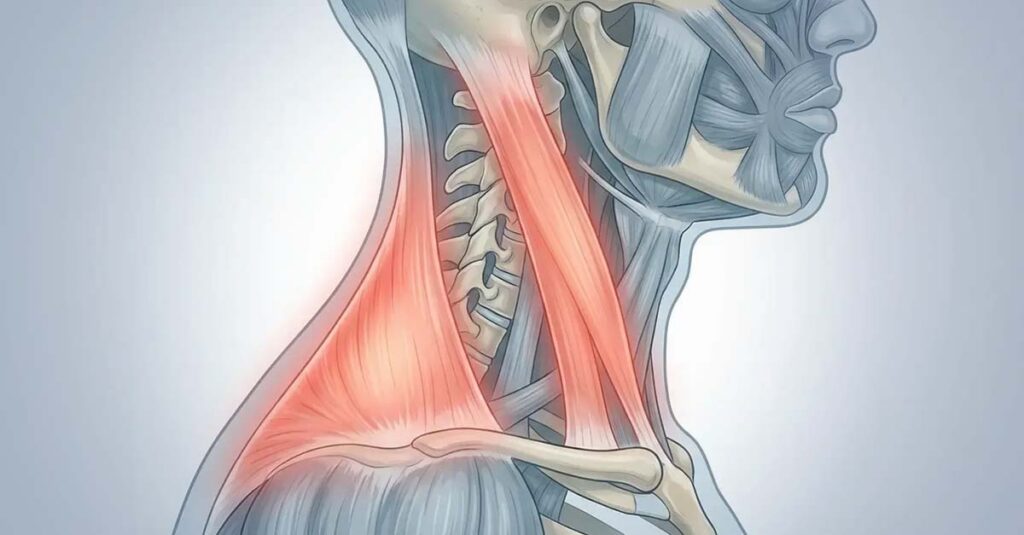
Cervical Strain
A cervical strain VA rating or neck strain VA rating typically falls under Diagnostic Code 5237. This is the most common classification for soft tissue injuries involving the muscles or tendons of the cervical spine—conditions that frequently result from carrying heavy equipment, whiplash injuries in vehicles, or acute trauma during physical training. Establishing a formal diagnosis under DC 5237 is the threshold requirement for this rating pathway.
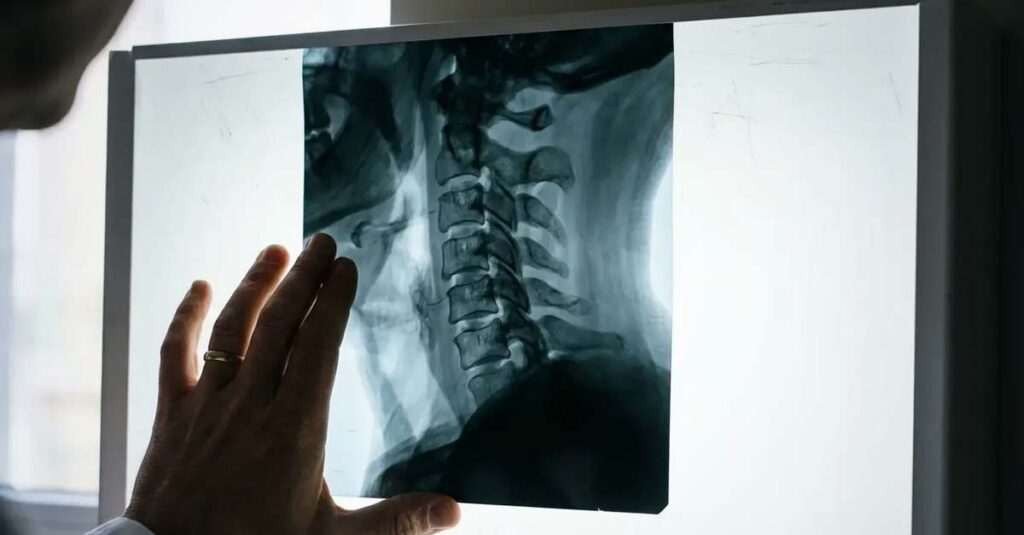
Degenerative Arthritis of the Cervical Spine
Rated under DC 5003, degenerative arthritis covers age-related or post-traumatic joint deterioration of the cervical spine. Veterans whose claims have been denied for lack of an identifiable acute injury should review whether imaging—including X-rays or MRI—reflects degenerative changes that support this alternative diagnostic pathway. Neck pain VA claims based on degeneration rather than discrete injury represent a valid and frequently overlooked route to service connection.
Establishing Service Connection
A diagnosis without a documented connection to military service does not produce a rating. The nexus—the causal link between the current disability and an in-service event—must be established before the severity of the condition becomes relevant. Understanding nexus letter VA: understanding independent medical opinions for service connection is essential for cases where the connection between service and the current condition is not self-evident from the service record.
Direct Service Connection
Direct service connection requires medical evidence of a specific in-service event or exposure that caused the current condition. Service treatment records documenting a cervical injury, combined with current imaging reflecting structural pathology at the same spinal level and an independent medical opinion establishing the causal relationship, constitute the strongest form of direct connection evidence.
A veteran who served as a paratrooper filed a claim for neck pain ten years after discharge. His service records included a documented entry reflecting neck stiffness following a hard parachute landing, at which time ibuprofen was prescribed. He combined this record with a current MRI showing a herniated disc at C5–C6 and an independent medical opinion from his treating physician stating the disc pathology was consistent with cumulative jump trauma. The VA granted service connection based on the documented in-service event, the current structural finding, and the clinical opinion linking the two.
Secondary Service Connection
When a service-connected condition—such as a lumbar spine disability or shoulder condition—has altered biomechanics or posture in a way that has caused or contributed to cervical spine pathology, a neck pain VA secondary claim may be supported. Documented mechanical compensation from a primary service-connected condition can establish the causal basis for a secondary cervical spine rating, supported by an independent medical opinion reflecting that relationship.
Aggravation
Veterans who had a pre-existing cervical condition documented on their entrance examination may still establish service connection if military duties permanently worsened the condition beyond its natural progression. The evidentiary standard for aggravation requires documentation that the worsening was attributable to service rather than the natural course of the disease.
The Mechanics of the VA Rating for Neck Pain
The VA disability rating for neck pain is governed by the General Rating Formula for Diseases and Injuries of the Spine. This formula is quantitative and criterion-based—it prioritizes measurable range of motion over subjective pain reports. Understanding the specific angular thresholds that define each rating tier is the foundation of an accurate cervical spine claim.
The General Rating Formula
VA Rating Criteria for Cervical Spine Conditions:
| Rating Percentage | Forward Flexion (Degrees) | Combined Range of Motion (Degrees) |
| 10% | 30° to 40° | 170° to 335° |
| 20% | 15° to 30° | 170° or less |
| 30% | 15° or less | N/A |
| 40% | Unfavorable ankylosis of the cervical spine | N/A |
| 100% | Unfavorable ankylosis of the entire spine | N/A |
A 10% rating is assigned when forward flexion is limited to between 30 and 40 degrees, or when combined range of motion is reduced to between 170 and 335 degrees. A 20% rating applies when forward flexion is between 15 and 30 degrees. These represent the most common ratings for veterans who retain some mobility but experience meaningful limitation. Higher ratings require more severe restriction, with a 30% rating requiring forward flexion of the cervical spine of 15 degrees or less, and 40% reserved for cases involving ankylosis.

Why Range of Motion Is the Primary Metric
The VA rating for neck range of motion is the central determinant of rating outcome. A difference of five degrees in forward flexion can produce a meaningful change in monthly compensation. This makes the accuracy of goniometric measurement—and the completeness of the examiner’s documentation—directly consequential to the veteran’s evaluation. Forward flexion, the movement of bringing the chin toward the chest, is the most heavily weighted component of the cervical spine evaluation and the metric most closely tied to the key rating thresholds.
Painful Motion as a Minimum Threshold
Under 38 CFR 4.59, the VA is required to assign a minimum compensable rating when motion in a joint is painful, even if the full range of motion is preserved. This regulatory provision protects veterans from receiving a 0% rating when their cervical spine moves through a normal arc but produces pain throughout or at the endpoint of movement. Pain during motion must be documented in the clinical record—specifically in the C&P examination report or DBQ—to activate this protection.
Functional Loss and Flare-Up Documentation
The VA is required under 38 CFR 4.40 and 4.45 to consider functional loss, including the degree of disability during flare-up episodes, when assigning a rating. A veteran whose cervical range of motion measures 35 degrees on the day of examination but who regularly experiences episodes in which spasm reduces flexion to 10 degrees for 48-hour periods should have that flare-up limitation reflected in the rating.
A veteran with a baseline forward flexion of 35 degrees experienced cervical spasms twice monthly that reduced her flexion to 10 degrees for approximately 48 hours per episode, during which she was unable to drive or perform tasks requiring downward gaze. Because her C&P exam coincided with a symptom-reduced period, she documented the flare-ups explicitly—specifying frequency, duration, and functional restrictions—which required the examiner to estimate range of motion loss during those episodes. The documented functional loss during flare-ups supported consideration for the higher 30% rating tier, and the VA evaluated her claim on that basis.
Bed Rest and Incapacitating Episodes
For veterans rated under DC 5243 (Intervertebral Disc Syndrome), an alternative rating pathway based on physician-prescribed bed rest is available. Six or more weeks of prescribed bed rest within a 12-month period supports a 60% rating under this code. This pathway is applicable when range of motion measurements alone do not reflect the true disability burden.
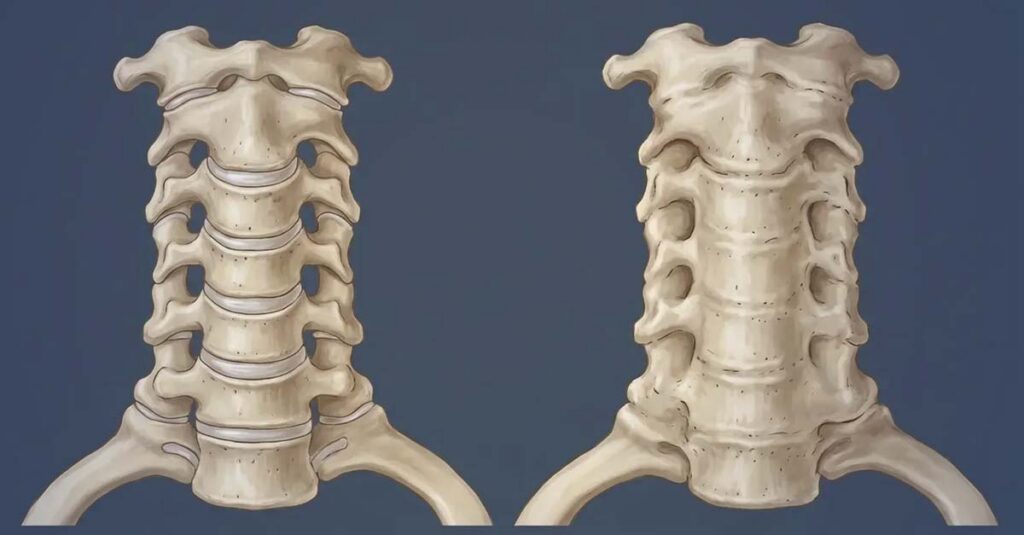
Ankylosis
Ankylosis—complete immobility of the cervical spine—produces the highest ratings under the General Rating Formula. Favorable ankylosis, where the joint is fixed in a neutral functional position, yields lower ratings than unfavorable ankylosis, where fixation occurs in a compromised or painful position. These ratings are reserved for the most severe cervical spine presentations.
The C&P Exam: Where the Rating Is Determined
The Compensation and Pension examination is the clinical event from which the rating is most directly derived. The examining physician’s documentation—particularly the completed DBQ—is the primary document the rating authority uses to assign a VA rating for neck pain. Understanding what the examiner is required to document, and what constitutes an incomplete or inaccurate examination, is essential preparation.
How the C&P Examination is Conducted
- Review personal medical records and prior DBQ documentation before the appointment
- Confirm that the examiner uses a goniometer to measure joint angles
- Prepare to describe flare-up episodes in specific terms: frequency, duration, and functional restrictions
- Stop range of motion movements at the point of pain onset—not at the point of maximum physical limitation
Goniometric Measurement
The examiner is required to use a goniometer—a calibrated protractor instrument—to measure cervical spine range of motion. Visual estimation of joint angles is not an acceptable substitute and may affect the accuracy of the examination findings. If a goniometer is not used during the C&P examination, the angular measurements recorded in the DBQ may be inaccurate, and the rating derived from those measurements may not reflect the true degree of limitation.

Repetitive Motion Testing
Per VA examination guidelines, the examiner must assess range of motion under repetitive-use conditions. If forward flexion measures 40 degrees on the first trial but decreases to 20 degrees on repeated attempts due to pain or fatigue, the reduced measurement should be the recorded metric. This distinction between initial and post-repetition range of motion is clinically significant and directly affects the applicable rating tier.
Describing Flare-Ups During the Exam
Because a C&P examination captures a single point in time, a veteran presenting on a symptom-reduced day risks a rating based on their best rather than typical functional status. Verbally describing the frequency, duration, and specific functional consequences of flare-up episodes—and ensuring those descriptions are incorporated into the examiner’s documentation—is the primary mechanism for preventing underrating in cervical spine claims.
The Disability Benefits Questionnaire
The DBQ for cervical spine conditions mirrors the General Rating Formula. It captures forward flexion measurements, combined range of motion, pain behavior, functional loss during flare-ups, and the presence of ankylosis or neurological deficits. Reviewing the VA DBQ process explained before the examination clarifies which clinical questions the examiner will be answering and helps ensure that all relevant information is communicated during the appointment.
Building a Complete Evidence File
Understanding the rating criteria is only useful when the clinical record reflects the evidence those criteria require. A claim that is well-documented and strategically organized substantially reduces the risk of an inaccurate rating based on incomplete information.
Medical Records
Collecting all private and military treatment records—with particular attention to documentation of cervical strain, stiffness, radiculopathy, or imaging findings—provides the objective evidentiary foundation of the claim. MRI and X-ray findings reflecting disc herniation, stenosis, or degenerative changes constitute objective evidence that supports and corroborates subjective symptom reports. For guidance on the full scope of documentation the VA considers, what evidence do I need for my disability claim provides a comprehensive reference.

Lay Statements
VA Form 21-10210 (Buddy Letter) submitted by a spouse, family member, or fellow service member provides lay observation evidence of the functional limitations caused by the cervical spine condition. Effective lay statements describe specific observable behaviors—such as the veteran’s inability to check blind spots while driving, difficulty performing overhead tasks, or the need to turn the entire torso to compensate for limited cervical rotation—rather than general characterizations of pain.
Buddy Letter Structure (VA Form 21-10210):
- Relationship: Identify the relationship to the veteran and the duration of that relationship
- Baseline: Describe the veteran’s physical condition and activity level prior to the injury or service period
- In-service observation (if applicable): Describe any witnessed incidents or physical changes observed during or following service
- Current functional observations: Document specific, observable limitations—include examples of activities the veteran avoids or modifies due to neck pain
- Frequency: Note how often observable symptoms or compensatory behaviors are witnessed
Symptom Logs
A 30-day symptom log maintained before filing—recording daily pain levels on a numeric scale, range of motion limitations during flare-up episodes, and specific functional restrictions—provides longitudinal evidence that a single examination cannot replicate. Documenting the frequency and functional impact of neck pain VA episodes creates a pattern of disability that supports accurate rating and counters the risk of underrating based on a single favorable exam day.
Secondary Claims and Filing
Filing accurately and identifying secondary conditions associated with the cervical spine disability ensures that the full scope of the service-connected impairment is evaluated.
Secondary Conditions Associated with Cervical Spine Disability:
| Secondary Condition | Connection to Neck Condition | Potential VA Rating |
| Cervical Radiculopathy | Nerve root compression causing arm pain, numbness, or weakness | 20%–40% per affected extremity |
| Migraines | Cervicogenic headaches triggered by cervical spine pathology | 0%–50% |
| Depression/Anxiety | Secondary mental health decline from chronic pain | 0%–100% |
| Sleep Apnea | Structural or medication-related aggravation | 0%–50% |
Filing the Initial Claim
When pursuing evaluation for a cervical spine condition, the medical documentation should clearly reflect the diagnosis and any related secondary conditions.
Cervical Radiculopathy
When neck pain radiates into the upper extremities—producing numbness, tingling, or weakness in the arms or hands—this reflects cervical radiculopathy secondary to the primary cervical spine condition. Radiculopathy is rated separately under the peripheral nerve rating schedule, with ratings available for each affected extremity. Veterans who have not filed for radiculopathy in addition to their cervical spine rating may have additional compensation potential that has not been evaluated.
Cervicogenic Migraines
Cervical spine pathology frequently produces cervicogenic headaches through referred pain and muscle tension mechanisms. When a pattern of headaches is temporally associated with cervical spine symptoms, a secondary claim for migraines may be supported by an independent medical opinion from a neurologist establishing the causal relationship. Reviewing the VA rating for migraines clarifies how headache conditions are evaluated and what documentation is required.
A veteran rated at 20% for cervical strain experienced frequent headaches that consistently coincided with cervical flare-up episodes. After maintaining a symptom log documenting the temporal relationship between cervical stiffness and headache onset, she filed a secondary claim for cervicogenic migraines supported by an independent neurological opinion reflecting the causal relationship. The VA awarded an additional 30% for migraines based on the documented evidence. The VA’s determination was based on the totality of the clinical record.

Accurate Documentation Through REE Medical
The VA rating for neck pain is directly dependent on the accuracy and completeness of the C&P examination. When the examiner does not use a goniometer, does not conduct repetitive motion testing, or does not document flare-up functional loss, the resulting rating may reflect an incomplete clinical picture rather than the veteran’s actual disability level.
REE Medical connects veterans with independent, licensed healthcare professionals who complete cervical spine DBQs and medical evaluations with the clinical thoroughness that an accurate VA disability rating for neck pain determination requires. Documentation coordinated through REE Medical is objective and VA-compliant, with specific attention to goniometric measurement accuracy, repetitive-use testing, flare-up functional loss documentation, and secondary condition identification. REE Medical operates on a flat-rate model—no percentage of future benefits is taken and pricing is transparent.
Veterans can learn more about coordinating independent medical documentation by contacting REE Medical for a complimentary informational consultation.
Final Thoughts
A VA rating for neck pain that accurately reflects cervical spine disability severity requires documentation that captures measurable range of motion, functional loss during flare-up episodes, and the secondary conditions that frequently accompany chronic cervical pathology. The General Rating Formula is objective and quantifiable—but only when the clinical record contains the specific angular measurements, repetitive-use findings, and flare-up documentation those criteria require.
Veterans who understand how forward flexion thresholds determine rating tiers, what examination procedures the VA is required to follow, and how to document the full functional burden of their cervical spine condition are substantially better positioned to receive compensation that reflects the actual impact of their service-connected disability.
DISCLAIMER: REE Medical, LLC is not a Veterans Service Organization (VSO) or a law firm and is not affiliated with the U.S. Veterans Administration (“VA”). Results are not guaranteed, and REE Medical, LLC makes no promises. REE Medical’s staff does not provide medical advice or legal advice, and REE Medical is not a law firm. Any information discussed, such as, but not limited to, the likely chance of an increase or service connection, estimated benefit amounts, and potential new ratings, is solely based on past client generalizations and not specific to any one patient. The doctor has the right to reject and/or refuse to complete a Veteran’s Disability Benefit Questionnaire if they feel the Veteran is not being truthful. The Veteran’s Administration is the only agency that can make a determination regarding whether or not a Veteran will receive an increase in their service-connected disabilities or make a decision on whether or not a disability will be considered service-connected. This business is not sponsored by, or affiliated with, the United States Department of Veterans Affairs, any State Department of Military and Veterans Affairs, or any other federally chartered veterans service organization.