Veteran Stress Management: The Comprehensive Guide to Reclaiming Your Peace
More than 3.3 million veterans have served in uniform since the September 11 attacks, each navigating a transition from the structured, purpose-driven environment of military service to a civilian landscape that frequently lacks the clarity, community, and mission that defined their identity. The stress that accompanies this transition is not simply psychological—it is physiological, administrative, relational, and occupational. Effective veteran stress management requires addressing all of these dimensions simultaneously.
This guide moves through the physiological roots of trauma and nervous system dysregulation, examines technological and lifestyle interventions grounded in current clinical evidence, addresses the often-overlooked administrative burden of the VA benefits process, and concludes with the family and workforce dynamics that shape post-service reintegration. The goal is a comprehensive framework that treats the veteran as a whole person operating within a complex environment—not a set of symptoms to be managed in isolation.
TL;DR
- Moral injury is distinct from PTSD: Shame and grief require different clinical approaches than fear-based trauma; identifying the correct category determines the effectiveness of treatment
- Bottom-up therapy addresses the root: Physically regulating the nervous system through somatic techniques often needs to occur before talk therapy can produce meaningful results
- Inflammation drives psychological symptoms: Gut health, sleep architecture, and anti-inflammatory nutrition are biological foundations for mental resilience, not peripheral lifestyle choices
- The VA process causes measurable stress: Institutional stress from the benefits system is real; outsourcing the documentation and claims process removes a significant and identifiable source of chronic anxiety
- Community is a clinical necessity: Isolation amplifies every other stressor; rebuilding a purpose-driven social structure is a biological requirement, not a social preference

The Physiological and Psychological Landscape
Veteran stress is rarely a purely psychological phenomenon. It is a systemic physiological event in which the nervous system remains locked in a chronic state of activation, unable to down-regulate despite the absence of immediate threat. Understanding the specific mechanisms driving this response—and distinguishing between different categories of stress—is the prerequisite for selecting interventions that are clinically appropriate.
Beyond PTSD: Moral Injury and Transition Stress
PTSD is the most widely recognized stress-related diagnosis in veteran populations, but it does not encompass the full range of post-service psychological distress. Many veterans experience conditions that PTSD-focused treatment frameworks were not designed to address. Understanding the nuances of these distinctions is essential for connecting with the right interventions; specific guidance on managing PTSD for veterans provides a useful foundation for distinguishing between general stress responses and clinical trauma presentations.
Moral Injury
Moral injury is a wound to the conscience produced by actions, witnessed events, or institutional betrayals that violated a person’s deeply held ethical framework. Neurologically, it engages the prefrontal cortex rather than the amygdala, manifesting as profound guilt, shame, or a sense of having been betrayed by leadership rather than as the fear-conditioned hyperarousal characteristic of PTSD. These are functionally different psychological states requiring different treatment modalities. Approaches centered on meaning-making, moral repair, and forgiveness are more clinically appropriate for moral injury than exposure-based therapies designed to extinguish fear responses.
The Loss of Tribe
Military service provides a high-trust, interdependent social environment in which individual identity is deeply embedded in collective purpose. Civilian life typically offers neither the density of trust nor the clarity of shared mission that characterize unit cohesion. This transition activates what journalist Sebastian Junger has described as a primal tribalism deficit—a biological stress response to social fragmentation that individual wellness practices alone cannot fully compensate for. Rebuilding a close-knit, purpose-oriented community is not a lifestyle preference; it is a clinical requirement for nervous system regulation and psychological stability.
Somatic and Nervous System Regulation
Cognitive behavioral approaches to stress operate from the top down—attempting to modify emotional and physiological states through thought and interpretation. For veterans whose nervous systems are chronically dysregulated, this approach often encounters a fundamental obstacle: the threat-detection systems of the brain operate faster than conscious cognition and are not amenable to rational override. Bottom-up somatic approaches—working directly with the body to produce physiological state change—frequently need to precede cognitive interventions for those interventions to be effective.
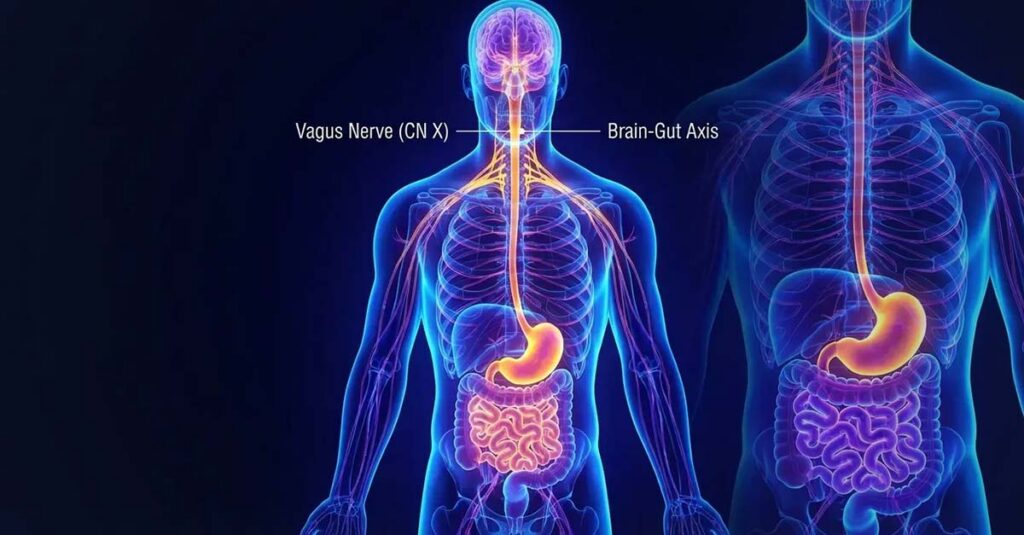
Polyvagal Theory in Practice
Polyvagal theory, developed by neuroscientist Stephen Porges, identifies a hierarchy of nervous system states—social engagement, mobilization, and immobilization—regulated by the vagus nerve. Chronic stress tends to suppress the social engagement state, leaving the nervous system defaulting to survival responses. Specific physical actions can directly stimulate vagal tone and restore access to the social engagement state without requiring cognitive processing.
The Physiological Sigh:
- Inhale deeply through the nose
- Take a second, shorter inhale through the nose to fully inflate the alveoli
- Exhale slowly and fully through the mouth
- Repeat three times to produce an immediate reduction in heart rate
This technique works by maximally inflating the lungs—which signals safety to the nervous system—followed by an extended exhale that activates the parasympathetic brake on cardiac output.
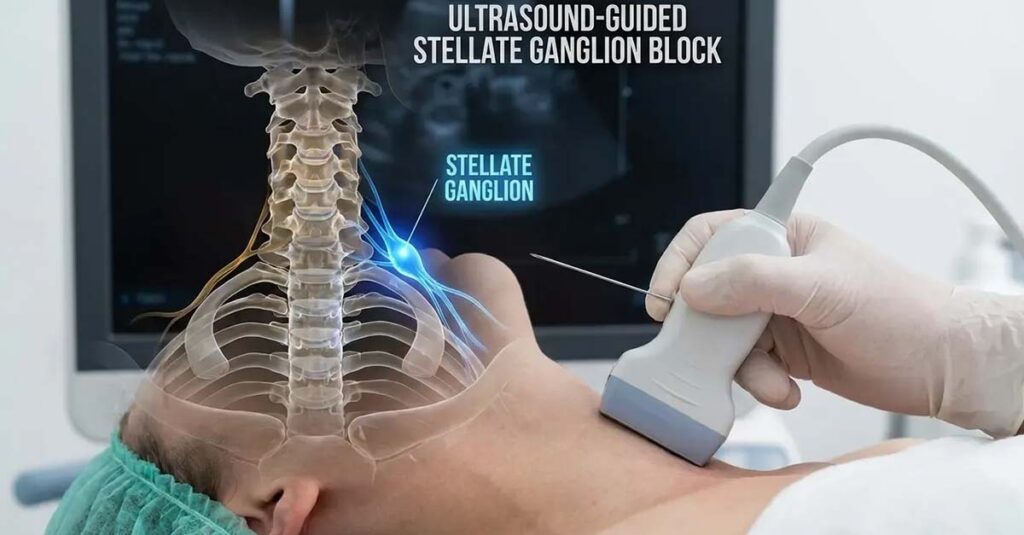
Stellate Ganglion Block
The Stellate Ganglion Block (SGB) is a clinical intervention that involves injecting a local anesthetic into a nerve cluster in the neck region of the sympathetic nervous system. Clinical research, including studies conducted within VA and military healthcare settings, indicates that SGB may produce significant reduction in hyperarousal symptoms associated with PTSD and chronic stress, providing a window of relative calm during which other therapeutic work can proceed. Veterans for whom conventional approaches have produced limited results may wish to discuss this option with a qualified physician.
Biofeedback
Biofeedback uses physiological sensors to display real-time data on heart rate variability, skin conductance, and other autonomic metrics, allowing individuals to observe and learn to influence their own stress responses. This approach transforms abstract concepts like relaxation into measurable, trainable outcomes. For veterans who respond well to data-driven, performance-oriented frameworks, biofeedback provides a concrete mechanism for developing voluntary regulation of the autonomic nervous system.
Technological and Lifestyle Interventions
The clinical landscape for veteran stress management has expanded substantially beyond pharmacological and conventional psychotherapeutic models. Precision health approaches, digital therapeutics, and evidence-based lifestyle interventions now offer veterans a range of tools for addressing the biological substrate of stress responses.

Digital Therapeutics and Virtual Reality
Virtual Reality Exposure Therapy
Virtual Reality Exposure Therapy (VRET) delivers graduated exposure to simulated stress-triggering environments—crowded marketplaces, highway driving, combat-adjacent scenarios—within a fully controlled clinical setting. This approach enables the brain to process and reconsolidate threatening stimuli without actual risk, progressively reducing the amplitude of the stress response associated with specific triggers. For veterans whose hypervigilance extends to environments that cannot be practically avoided in civilian life, VRET provides a clinical precision that conventional imaginal exposure cannot replicate.
Wearable Stress Tracking
Devices such as Oura and WHOOP quantify allostatic load—the cumulative physiological cost of sustained stress exposure. By monitoring metrics including heart rate variability, resting heart rate, sleep efficiency, and skin temperature trends, these devices enable early identification of physiological depletion before it manifests as psychological crisis.
Comparative Analysis of Key Stress Metrics in Wearable Devices:
| Metric | What It Measures | Relevance for Veterans |
| HRV (Heart Rate Variability) | Variation in time between heartbeats | High HRV indicates a recovered nervous system; low HRV signals sympathetic dominance |
| RHR (Resting Heart Rate) | Beats per minute at complete rest | A rising RHR often precedes burnout or emotional difficulty before subjective awareness |
| Sleep Efficiency | Percentage of time in bed actually spent asleep | Fragmented sleep is a primary driver of hypervigilance and irritability |
| Skin Temperature | Surface body temperature trends | Deviations can signal the onset of stress-induced immune activation |
Functional Medicine and Nutrition
The Gut-Brain Axis
Approximately 95% of the body’s serotonin is produced in the gastrointestinal tract. Chronic stress degrades gut microbiome diversity and intestinal barrier integrity, which in turn disrupts serotonin production and increases systemic inflammation—creating a bidirectional feedback loop in which stress damages gut health and compromised gut health worsens psychological resilience. Targeted probiotic supplementation and reduction of primary inflammatory dietary inputs constitute a meaningful biological intervention for mood stabilization.

Sleep Architecture and CBT-I
Sleep deprivation is among the most powerful amplifiers of hypervigilance, emotional reactivity, and stress sensitivity. Cognitive Behavioral Therapy for Insomnia (CBT-I) techniques, including sleep restriction therapy and stimulus control, systematically address the conditioned arousal that prevents restorative sleep in veterans with chronic insomnia.
Veteran Sleep Hygiene Checklist:
- No caffeine within 10 hours of intended sleep time
- Bedroom temperature set to 65–67°F to facilitate core temperature drop
- No blue-light exposure from screens within 60 minutes of sleep
- If not asleep within 20 minutes, leave the bed and engage in low-stimulation activity until sleepy
- Use white noise or a fan to mask environmental sounds that activate the threat-detection response
Anti-Inflammatory Nutrition
Neuroinflammation has an established relationship with depressive and anxiety symptoms. Diets high in omega-3 fatty acids, polyphenols, and fiber—and low in refined carbohydrates and ultra-processed foods—reduce the inflammatory load on the central nervous system. Baseline inflammatory markers, including C-Reactive Protein, can be measured through routine blood work and tracked over time to assess the impact of dietary changes.
Adaptive Exercise
For veterans with dysregulated stress responses, high-intensity exercise protocols that produce significant cortisol spikes may temporarily worsen hyperarousal symptoms. Adaptive exercise approaches—including rucking, swimming, and other rhythmic, moderate-intensity activities—metabolize circulating stress hormones without activating the physiological arousal pattern associated with high-intensity training. These protocols support veteran stress management by reducing the physiological substrate of anxiety while building physical capacity.

Community and Peer Support
Isolation is a primary amplifier of every other stressor in the post-service environment. Modern peer support frameworks have evolved toward structured, accountability-based models organized around shared purpose and meaningful action. Mental health support and finding strength in veteran connections is often among the most effective interventions for combating the social fragmentation of civilian life.
Veteran Service Organizations that have shifted toward active community service and physical challenge events leverage the helper principle—the well-documented psychological benefit of providing meaningful assistance to others. Active engagement in mission-driven service reduces personal stress by restoring the sense of purpose and contribution that military service provided.
Navigating Systemic and Administrative Stressors
The VA benefits process is a substantial and frequently underrecognized source of chronic stress for veterans. The structure of the claims process, extended wait times, and the experience of feeling dismissed during examinations can produce what clinicians describe as institutional stress—a distinct response generated by the bureaucratic systems designed to provide support.
Financial Stability and the Claims Process
Financial instability is one of the most direct contributors to chronic psychological stress. A veteran living with an undertreated or underrated disability carries both the physical burden of the condition and the financial pressure of inadequate compensation—a combination that sustains background anxiety regardless of how effectively other stress management strategies are applied. Securing an accurate VA disability rating addresses a specific and measurable stressor: it establishes the material security that supports engagement in other aspects of recovery. Understanding the specific criteria for a VA rating for anxiety is a practical first step for veterans whose stress has produced clinically significant symptoms.
Documentation Accuracy in C&P Examinations
Compensation and Pension examinations are consequential clinical events. When a veteran feels rushed or insufficiently evaluated, the resulting documentation may not accurately reflect functional limitations—producing an underrated disability and sustained financial and psychological burden. Independent medical documentation prepared outside the C&P examination framework provides an alternative evidentiary record that the VA is required to consider.
Managing the Wait
Extended wait times for VA decisions create sustained uncertainty that maintains stress activation throughout the review period. Having complete medical documentation in place before submission can help reduce uncertainty during the review period.
Structured vs. Unstructured Claims Management:
A veteran who submits a claim without independent supporting documentation and monitors the VA application portal daily experiences status-related anxiety throughout the review period. A veteran with complete medical documentation may feel more confident in the evidence less claims-related stress during the review period.

REE Medical and Administrative Stress
REE Medical connects veterans with independent, licensed medical professionals who complete Disability Benefits Questionnaires with clinical thoroughness and disability-specific expertise. When the medical documentation accurately reflects the full scope of a veteran’s condition, the claims process becomes a matter of confident submission rather than an ongoing administrative burden. This removes both the financial uncertainty and the psychological weight of navigating the system without adequate medical support. REE Medical operates on a flat-rate model with transparent pricing; no percentage of future benefits is taken.
The Ecosystem of Reintegration: Family and Workforce
Stress management strategies that address only the individual veteran without accounting for the family system and professional environment in which that veteran operates are structurally incomplete. The stress of post-service life is distributed across households and careers.
Secondary Trauma and Family Dynamics
Family members of veterans with chronic stress or trauma-related conditions frequently experience Secondary Traumatic Stress—a measurable physiological and psychological response to sustained proximity to another person’s distress. This is a biological reality that requires structured support, not a personal failing.

Compassion Fatigue in Partners and Caregivers
Partners who absorb the primary emotional and logistical management of a veteran’s post-service stress experience progressive depletion of their own empathic capacity—a clinical phenomenon known as compassion fatigue. Scheduled respite—structured time for partners to disengage from the caregiver role and restore their own psychological resources—is a clinical necessity for the long-term sustainability of the caregiving relationship.
Naming the Weather
Families of veterans with stress-related conditions often develop a mirroring hypervigilance—monitoring the veteran’s emotional state and adjusting household behavior accordingly. A communication practice of explicitly acknowledging the veteran’s current emotional state without the family accepting responsibility for resolving it creates a more honest and less tension-laden household dynamic.

Professional Identity and Workforce Stress
The Authority Gap
Military authority is positional—vested in rank and formalized through command structure. Civilian organizational authority is largely relational—derived from influence, demonstrated competence, and interpersonal capital built over time. Developing the capacity to achieve organizational outcomes through persuasion, relationship-building, and demonstrated value is among the most practically important professional skills for reducing workplace friction during post-service career development.
Translating Military Competencies
Veterans are trained as expert generalists capable of leading teams, managing complex logistics, and maintaining accountability for high-value assets. Civilian hiring processes are predominantly structured around specialist credentials and role-specific technical skills. The mismatch between veterans’ actual capability and how that capability is communicated in civilian resume formats is a significant source of job search stress that can be directly addressed through systematic skills translation. Tips for a smooth transition to civilian life can help veterans translate their competencies effectively and reduce career-related stress.
Military to Civilian Competency Translation:
| Military Concept | Civilian Resume Language |
| NCOIC / Squad Leader | “Operations Manager overseeing cross-functional teams of 10+ personnel” |
| Mission Accomplishment | “Project Management: Delivered complex initiatives on time and under budget” |
| OpOrder / Briefings | “Strategic Communication: Presented data-driven reports to executive leadership” |
| Property Accountability | “Asset Management: Maintained 100% accountability of $2M+ in inventory” |
Resume Rewrite Example:
- Military: “Responsible for the health and welfare of 40 soldiers and $10M in equipment”
- Civilian: “Directed HR and logistical operations for a 40-person department, maintaining zero loss rate for $10M in assets while reducing personnel turnover by 15%”
Finding Purpose Beyond Rank
The loss of a clearly defined mission is among the most psychologically destabilizing aspects of the military-to-civilian transition. Veterans who do not replace the mission-driven structure of service with an equivalently purposeful civilian endeavor frequently experience identity diffusion that amplifies other stressors. Entrepreneurship, mentorship, community leadership, and advocacy work each provide frameworks within which high-drive, mission-oriented individuals can channel their capacity for commitment and organizational execution toward meaningful outcomes.

Final Thoughts
Effective veteran stress management is a multi-domain undertaking. It requires regulating the nervous system through somatic and clinical interventions, addressing the biological substrate of stress through nutrition and sleep, securing the financial stability that accurate VA compensation provides, rebuilding the community structures that military service made available, and navigating the family and workforce dynamics of civilian reintegration.
These domains are not independent—they are mutually reinforcing. Financial instability sustained by an inaccurate VA rating undermines sleep, which degrades nervous system regulation, which strains family relationships, which amplifies workplace stress. Conversely, accurate documentation that produces appropriate compensation removes a specific and identifiable stressor, creating space for every other intervention to gain traction.
Veterans do not have to accept chronic hypervigilance as the permanent cost of service. The tools, frameworks, and support systems required for a post-service life defined by purpose rather than by the residue of stress and trauma are accessible—but accessing them requires a comprehensive strategy rather than isolated interventions applied to individual symptoms.
DISCLAIMER: REE Medical, LLC is not a Veterans Service Organization (VSO) or a law firm and is not affiliated with the U.S. Veterans Administration (“VA”). Results are not guaranteed, and REE Medical, LLC makes no promises. REE Medical’s staff does not provide medical advice or legal advice, and REE Medical is not a law firm. Any information discussed, such as, but not limited to, the likely chance of an increase or service connection, estimated benefit amounts, and potential new ratings, is solely based on past client generalizations and not specific to any one patient. The doctor has the right to reject and/or refuse to complete a Veteran’s Disability Benefit Questionnaire if they feel the Veteran is not being truthful. The Veteran’s Administration is the only agency that can make a determination regarding whether or not a Veteran will receive an increase in their service-connected disabilities or make a decision on whether or not a disability will be considered service-connected. This business is not sponsored by, or affiliated with, the United States Department of Veterans Affairs, any State Department of Military and Veterans Affairs, or any other federally chartered veterans service organization.