Heart Health Tips for Veterans: The Silent Danger Your Doctor Might Miss
Veterans carry more than memories from their time in service. The physical toll of military life—toxic exposures, chronic pain, high-stress environments, and disrupted sleep—creates a cardiovascular profile that standard medical advice rarely accounts for. Generic guidance to “eat better and exercise more” fails to address the complex, service-connected factors that silently shape a veteran’s long-term heart health.
This guide explores the environmental, physical, and psychological contributors that are most frequently overlooked in veteran cardiovascular care. It also outlines practical, realistic strategies adapted to the realities of life after service, along with the advanced diagnostics and documentation that allow the VA to accurately evaluate the full scope of these conditions.
Why Your Heart Tells a Different Story
Standard heart health advice is designed for the general population. It does not account for the metabolic demands of combat environments, the physiological aftermath of chemical exposure, or the chronic systemic stress that follows years of high-stakes military service. Applying heart health tips for veterans effectively begins with understanding the unique variables that shaped cardiovascular health during service.
Military life introduces physiological risk factors that civilians simply do not encounter. From accelerated arterial hardening caused by herbicide exposure to the autonomic disruption caused by PTSD, a veteran’s heart reflects the cumulative history of their service. Meaningful management of that health begins with recognizing where those risks originated.
Environmental Hazards You Can’t Outrun
A clean diet and favorable genetics do not eliminate cardiovascular risk for veterans who were exposed to specific environmental hazards during deployment. These exposures often act as silent, long-term antagonists to heart health—making targeted screening and thorough medical documentation essential components of any cardiovascular evaluation.
Chemical Exposures
Toxic exposure is not solely a respiratory issue. The chemicals encountered during service can alter the lining of blood vessels long after a veteran has left the theater of operations, creating vascular damage that may manifest years—or even decades—later.
Legislative milestones like the PACT Act have formally acknowledged that toxic exposure creates long-term systemic issues, validating what many veterans have understood about their health for years. That acknowledgment has significant implications for how cardiovascular conditions are documented and evaluated within the VA system.
Agent Orange and Your Arteries
For veterans who served in Vietnam or other areas with documented herbicide use, the connection between Agent Orange exposure and Ischemic Heart Disease is recognized as presumptive by the VA. These chemicals accelerate arterial hardening—a process that may be well underway even in veterans who are currently asymptomatic. Early arterial screening, rather than a standard pulse check, is the appropriate clinical response to this type of exposure history.
The Burn Pit Legacy
Particulate matter from burn pits and sandstorms in Southwest Asia does more than damage the lungs. Inhaling these toxins triggers a state of chronic inflammation that stresses the entire cardiovascular system. Over decades, that silent inflammation can drive up blood pressure and stroke risk in ways that standard clinical assessments may not detect without specialized testing.

When Pain Stops You From Moving
Chronic pain from musculoskeletal injuries creates a substantial barrier to traditional cardiovascular exercise—and that barrier has direct consequences for heart health. The intersection of physical injury and cardiac risk requires a modified, injury-aware approach to physical activity.
The Physical Toll of Service
Musculoskeletal injuries are among the most common service-connected disabilities, and their cardiovascular impact extends well beyond orthopedic function. The relationship between chronic back pain, hip injuries, and elevated blood pressure is well-documented, yet frequently overlooked in routine medical evaluations.
The Inactivity Trap
Injuries to hips, knees, and the spine frequently impose a sedentary lifestyle—not out of choice, but out of necessity. Inactivity weakens the heart muscle and contributes to weight gain, which then places additional mechanical stress on the same joints responsible for limiting movement. Breaking this cycle requires a deliberate, injury-aware approach to physical activity.
Inflammation Highways
Pain is typically a signal of inflammation—but that inflammation does not remain localized. Systemic inflammation travels through the bloodstream, damaging blood vessel linings and promoting the buildup of arterial plaque. An injury may be local in origin, but its inflammatory consequences are systemic in scope.
The NSAID Problem
Long-term reliance on ibuprofen and other NSAIDs to manage chronic pain is common in the veteran population, but it carries meaningful cardiovascular risks. Extended use can elevate blood pressure and increase the risk of heart failure. Heart-safe pain management alternatives are available and worth discussing with a treating physician.

Real World Tactics for Better Health
Effective heart health tips for veterans account for the physical and logistical realities of life after service. The following strategies are practical adaptations that work within the constraints many veterans navigate daily.
Eating Like a Civilian
Transitioning from high-calorie military rations and mess hall food to a civilian diet requires significant adjustment. A restrictive approach often fails. An additive nutrition strategy—focusing on what beneficial foods can be incorporated rather than what must be eliminated—tends to be more sustainable and more effective for long-term cardiovascular health.
Retraining the Salt Tooth
Military rations are heavily preserved with sodium, and years of consuming them can significantly desensitize the palate. Gradual substitution of high-sodium staples with potassium-rich herbs and spices allows taste preferences to adjust over time, supporting lower blood pressure without sacrificing flavor.

The Crowding Out Strategy
Rather than eliminating comfort foods outright, a “crowding out” approach focuses on consuming fiber-rich vegetables first during a meal. This regulates blood sugar, promotes satiety, and naturally reduces the volume of less nutritious food consumed—without triggering the psychological resistance that comes with deprivation-based dieting.
Practical Application: Rather than eliminating pizza night, consuming a large bowl of spinach salad with olive oil and vinegar before the first slice allows fiber to create satiety earlier in the meal. The likely result is satisfaction after two slices rather than four—naturally reducing caloric and sodium intake without a formal dietary restriction.
Exercise That Doesn’t Wreck Your Knees
Sustainable cardiovascular exercise is exercise that can be maintained over time. For veterans managing service-connected disabilities, the goal is elevating heart rate without compounding joint damage. Fitness resources for veterans of all abilities outline adaptive routines that protect joints while strengthening the cardiovascular system.
High Intensity, Low Impact
Battle ropes, rowing machines, and swimming deliver meaningful cardiovascular benefits without the concussive force that running places on the spine and knees. These modalities are effective alternatives for veterans whose lower-body joints cannot tolerate high-impact training.
Rucking Light
Rucking with a significantly reduced load—or no load at all—maintains cardiovascular endurance while preserving the psychological familiarity of a routine many veterans valued during service. Reducing the weight removes the primary mechanical stressor on the spine and knees while keeping the cardiovascular benefit largely intact.

Zone 2 Training
Training at approximately 60–70% of maximum heart rate—commonly referred to as Zone 2—builds mitochondrial efficiency and improves long-term heart health without the physical stress associated with high-intensity interval training. This approach is particularly well-suited for veterans managing chronic pain or recovering from orthopedic injuries.
Ditching the Crutches
Tobacco and alcohol are deeply embedded in military culture as stress management tools. Both are primary cardiovascular risk factors with well-documented effects on blood pressure, arterial health, and cardiac function.
Nicotine and Stress
Nicotine is commonly used as an anxiety management mechanism. Successful cessation typically involves replacing the behavioral ritual of smoking with an alternative stress-relief habit. Breathing exercises and tactile tools address the underlying stress response without the blood pressure consequences associated with continued nicotine use.

The Brain-Heart Connection
The heart and brain are physiologically interconnected systems. Mental health conditions such as PTSD, anxiety, and depression are not purely psychological experiences—they are active physiological stressors that degrade cardiovascular function over time. Addressing mental health is, in a measurable clinical sense, addressing heart health.
PTSD and Physiology
Post-Traumatic Stress Disorder maintains the body in a state of chronic hyperarousal, with direct consequences for cardiac rhythm and long-term heart function. Managing PTSD is not solely a mental health priority—it is a critical component of preventing long-term cardiac damage, because the body’s stress response does not distinguish between psychological and physical threats.
Stuck in Fight or Flight
A permanently elevated fight-or-flight state floods the body with cortisol and adrenaline, keeping blood pressure chronically elevated and progressively damaging arterial walls. The threat triggering this response may not be physically present, but the cardiovascular damage it produces is real and cumulative.

Heart Rate Variability
A healthy heart exhibits subtle rhythmic variation in response to breathing and physical activity—a measure known as Heart Rate Variability (HRV). PTSD is clinically associated with low HRV, which indicates a heart under sustained stress with reduced capacity to adapt to physical demands. Low HRV is a recognized predictor of future cardiac events.
Hypervigilance Burnout
Sustained hypervigilance consumes significant metabolic resources and keeps heart rate elevated even during periods of rest. Over time, this persistent high-idle state contributes to premature cardiac fatigue, as the cardiovascular system operates at a chronically elevated baseline.
Ignoring the Signs
Emotional numbing is a common psychological coping mechanism that can lead to the dismissal of physical warning signals such as chest tightness or shortness of breath. Delayed recognition of these symptoms leads to delayed clinical intervention—a pattern with serious cardiovascular consequences.

The Battle for Sleep
Sleep is the period during which the cardiovascular system undergoes critical repair. Veterans disproportionately experience sleep disturbances that deprive the heart of this essential recovery window, compounding cardiovascular risk over time.
Sleep Apnea
Obstructive Sleep Apnea (OSA) is prevalent in the veteran population. When left untreated, OSA causes nocturnal oxygen levels to drop repeatedly throughout the night, forcing the heart to pump harder to compensate. This is a well-documented driver of secondary hypertension.
Nightmares
Service-related nightmares trigger adrenaline spikes during sleep, keeping the heart in an elevated state even during rest hours. This prevents the blood pressure “dipping” that normally occurs overnight—a physiological process that provides the vascular system with a period of reduced mechanical stress.

Isolation Kills
The transition to civilian life frequently severs the close social bonds formed during service. Social isolation carries cardiovascular risk that research has compared in magnitude to that of smoking, making community an active component of heart health—not simply a quality-of-life consideration.
Loneliness Physiology
Isolation activates a survival response in the brain that increases both systemic inflammation and blood pressure. Rebuilding meaningful social connection—whether through a veteran-specific organization, a community group, or a shared hobby—functions as a tangible medical intervention with measurable cardiovascular benefits.
Finding a Health Battle Buddy
The accountability structures inherent in military culture have direct applicability to health maintenance. A peer-based “health battle buddy” system—in which veterans regularly check in on one another’s blood pressure readings, medication adherence, or exercise consistency—leverages existing behavioral conditioning to support long-term health adherence.
Service as Medicine
Engagement in service-oriented volunteering restores a sense of purpose that many veterans lose during the transition to civilian life. Research supports that altruistic behavior reduces stress hormone levels and blood pressure, producing a measurable protective effect on cardiovascular health.
Fighting the Medical Bureaucracy
Managing cardiovascular health as a veteran means navigating a medical system that standard annual check-ups are often insufficient to address. The specific cardiovascular markers most relevant to veteran health require proactive screening and thorough, consistent documentation.
Tests Your Doctor Might Skip
Standard cholesterol panels frequently miss the cardiovascular risk profile most relevant to veterans. Normal cholesterol does not indicate normal cardiovascular risk when systemic inflammation or arterial calcification is present. The following advanced diagnostics are particularly relevant for the veteran population:
Veterans Cardiology Checklist:
- Lipoprotein(a) Test: Screens for a genetic cholesterol variant frequently associated with cardiac events but rarely included in standard panels.
- Hs-CRP (High-Sensitivity C-Reactive Protein): Measures systemic inflammation levels, which are often elevated in the presence of PTSD or chronic pain.
- Coronary Artery Calcium (CAC) Scan: A CT-based imaging tool that visualizes hard plaque buildup within the arteries.
- ApoB Test: Often a more accurate predictor of cardiovascular disease risk than standard LDL cholesterol measurement.
- Sleep Study (Polysomnography): Clinically evaluates sleep apnea as a potential driver of hypertension.
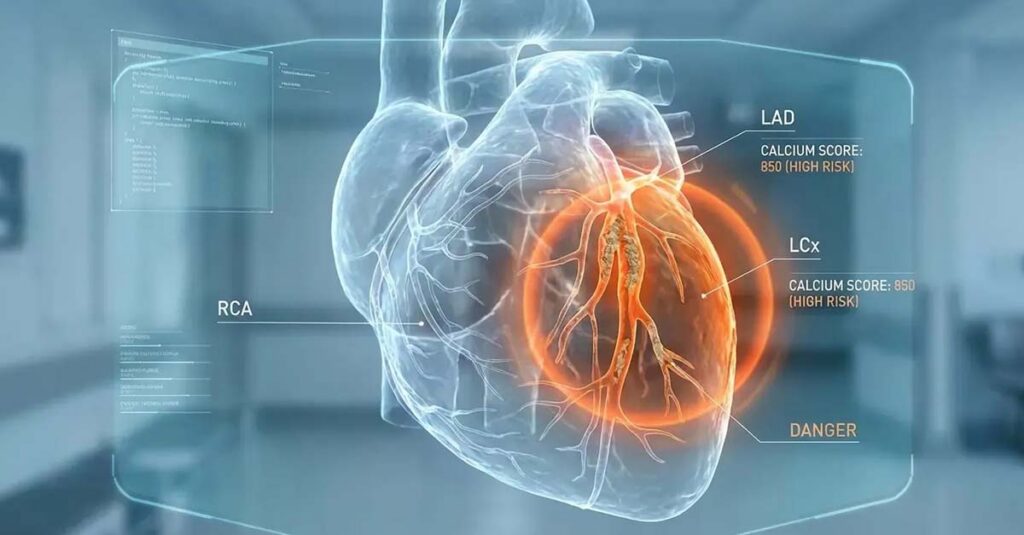
Calcium Scoring
A Coronary Artery Calcium (CAC) scan detects calcium deposits in the arterial walls, providing direct visualization of early-stage atherosclerosis. For veterans with a history of Agent Orange or burn pit exposure, this test offers detection capability years before comparable findings would appear on a standard stress test.
Inflammation Markers
Because chronic pain and PTSD both drive systemic inflammation, High-Sensitivity C-Reactive Protein (hs-CRP) testing is a particularly relevant diagnostic tool for veterans. This test measures general inflammatory burden and predicts cardiovascular disease risk even in individuals whose cholesterol and blood pressure readings appear within normal ranges.
24-Hour BP Monitoring
In-office blood pressure readings can be skewed by clinical anxiety—a dynamic that affects many veterans in VA settings. Ambulatory blood pressure monitoring involves wearing a cuff for 24 hours, capturing readings across daily activities and sleep. This method produces a more comprehensive picture of true cardiovascular load than a single clinical reading can reflect.
When ambulatory readings consistently reflect elevated patterns, the criteria for VA rating for hypertension describe how the VA evaluates that evidence within the claims process.
Imaging Stress Tests
A standard exercise stress test may not detect subtle blockages and requires physical exertion that veterans with significant orthopedic injuries may not be able to perform safely. A pharmacologic stress test—or one conducted with concurrent echocardiogram imaging—can accurately assess cardiac function regardless of physical mobility limitations.

Paperwork Saves Lives
In veteran healthcare, documentation is the mechanism through which a medical condition becomes formally recognized and accurately evaluated. Comprehensive medical records are what allow the VA to assess the full scope of a veteran’s condition.
The Independent Medical Opinion
Establishing a clinical connection between a heart condition and military service typically involves an independent medical opinion—a formal statement prepared by a licensed medical professional indicating that a condition is medically linked to service. The importance of thorough medical evidence in the VA evaluation process is well-documented, and comprehensive clinical records are foundational to accurate VA assessment.
A medical provider may document whether a condition is related to military service based on their clinical judgment and review of medical history
Symptom Logging
A detailed log of cardiac symptoms—recorded alongside their triggers—allows subjective experiences to become part of the objective medical record. Noting when palpitations occur in relation to a high-pain day or a nighttime episode provides clinical context that episodic office visits alone cannot capture.

How REE Medical Supports Accurate Documentation
Many cardiovascular conditions in veterans are secondary to service-connected disabilities such as PTSD, sleep apnea, or chronic pain. The nuance of those clinical connections is not always reflected in initial VA evaluations, particularly when medical documentation lacks the specificity required to describe the full scope of a condition.
REE Medical connects veterans with independent, licensed healthcare professionals who complete detailed Disability Benefits Questionnaires (DBQs) and medical evaluations that meet VA formatting standards. Providers are experienced with disability-focused documentation and VA-standardized forms. REE Medical does not prepare, present, or submit VA disability claims and does not provide legal or representational services.
Accurate documentation that clearly reflects the severity and service connection of a cardiovascular condition allows the VA to conduct a thorough and informed evaluation. A disability rating that reflects the true clinical picture provides the financial foundation necessary to access improved nutrition, consistent medical care, and reduced financial stress—all of which are meaningful contributors to long-term cardiovascular health.
Veterans can learn more about coordinating independent, VA-compliant medical evaluations by contacting REE Medical for an informational consultation.
Final Thoughts
Protecting cardiovascular health as a veteran requires more than routine check-ups and standard lifestyle modifications. It requires an understanding of the specific exposures, injuries, and psychological conditions that define a veteran’s health history—and access to diagnostics and documentation that reflect that complexity.
A disability rating that accurately reflects the severity of service-connected conditions provides the resources necessary to meaningfully address cardiovascular risk. Whether the concern is hypertension connected to PTSD, atherosclerosis linked to toxic exposure, or cardiac risk compounded by chronic pain and inactivity, complete and accurate clinical documentation is the foundation of an informed VA evaluation.
Staying informed on heart health for heroes is a lifelong commitment—and with the right medical documentation, appropriate diagnostics, and a clear understanding of the service-connected factors at play, it is a challenge the veteran community is well-equipped to meet.
DISCLAIMER: REE Medical, LLC is not a Veterans Service Organization (VSO) or a law firm and is not affiliated with the U.S. Veterans Administration (“VA”). Results are not guaranteed, and REE Medical, LLC makes no promises. REE Medical’s staff does not provide medical advice or legal advice, and REE Medical is not a law firm. Any information discussed, such as, but not limited to, the likely chance of an increase or service connection, estimated benefit amounts, and potential new ratings, is solely based on past client generalizations and not specific to any one patient. The doctor has the right to reject and/or refuse to complete a Veteran’s Disability Benefit Questionnaire if they feel the Veteran is not being truthful. The Veteran’s Administration is the only agency that can make a determination regarding whether or not a Veteran will receive an increase in their service-connected disabilities or make a decision on whether or not a disability will be considered service-connected. This business is not sponsored by, or affiliated with, the United States Department of Veterans Affairs, any State Department of Military and Veterans Affairs, or any other federally chartered veterans service organization.