Veteran Mental Health Support Has Changed: Why Your Old Diagnosis Might Be Wrong
The mental health landscape for veterans has shifted dramatically in the past decade. What was once understood as a straightforward case of post-traumatic stress disorder may actually be moral injury, identity loss, chronic inflammation, or traumatic brain injury—conditions that demand entirely different treatment approaches. The science has evolved, but many veterans remain locked into outdated diagnostic frameworks that fail to capture the full complexity of post-service psychological distress. Understanding these distinctions isn’t just about getting the right therapy; it’s about ensuring the medical documentation accurately reflects the severity and origin of symptoms, which directly impacts access to sustained care and financial support through the VA disability system.
TL;DR
PTSD is too narrow a label. Many veterans experience moral injury or identity loss, which requires different treatment than standard fear-based trauma. Physical health drives mental health. Inflammation, sleep disruption, and hormonal imbalances often mimic depression and anxiety. Women veterans need specialized care. Military Sexual Trauma (MST) involves betrayal by peers, necessitating a focus on trust-building before trauma processing. New therapies are emerging. Stellate Ganglion Blocks (SGB), TMS, and psychedelic-assisted therapies offer hope where traditional medications fail. Documentation is critical. Access to comprehensive care often depends on accurate Disability Benefits Questionnaires (DBQs) and independent medical opinions that clearly describe functional impairment and symptom origin.

Why “Just PTSD” Doesn’t Cut It Anymore
The system has historically viewed veteran psychological distress through the single lens of PTSD. For decades, diagnostic criteria focused on a rigid definition involving flashbacks, hypervigilance, and anxiety rooted in life-threatening events. Current research demonstrates that distress is far more nuanced, involving loss of purpose, deep-seated moral conflicts, and physiological changes that occur after combat. An estimated 41% of veterans require mental health support programs every year, yet misidentifying the root cause often leads to ineffective treatment plans. Documenting symptoms that don’t fit the standard PTSD mold—such as feelings of betrayal, existential emptiness, or cognitive difficulties—allows providers to understand the full scope of the condition and ensures the VA can accurately assess functional impairment.
It’s Not Always Fear: Moral Injury and Transition Stress
Not every psychological struggle stems from a near-death experience. A substantial amount of suffering originates from “moral injury” and “transition stress,” which are distinct from PTSD. Transition stress represents the decompression experience of leaving a high-structure military environment for a chaotic civilian world. Recognizing the difference between fear-based trauma and conscience-based injury is the first step toward accurate diagnosis and appropriate treatment. While identifying these distinctions is crucial for treatment planning, understanding how the VA categorizes these different stressors is also important for disability claims; veterans can read more about understanding VA disability benefits for PTSD to see how the VA evaluates these conditions.
| Feature | Post-Traumatic Stress Disorder (PTSD) | Moral Injury |
| Primary Emotion | Fear, Horror, Helplessness | Guilt, Shame, Anger, Disgust |
| Trigger | Actual or threatened death/injury | Acts that violate deep moral beliefs |
| Core Mechanism | Hyperarousal (Fight or Flight) | Broken Trust (in self or authority) |
| Physiological Response | Adrenaline spikes, panic attacks | Heaviness, withdrawal, depression |
| Treatment Focus | Extinguishing fear response (PE, CPT) | Rebuilding trust, forgiveness, making amends |
When Your Conscience Takes the Hit
Moral injury occurs when individuals witness, fail to prevent, or participate in acts that violate core moral beliefs. While PTSD is rooted in fear, moral injury is rooted in shame, guilt, and broken trust. A violation of the soul cannot be treated with the same protocols used for a fear response. The VA’s National Center for PTSD describes moral injury as “the distressing psychological, behavioral, social, and sometimes spiritual aftermath of exposure to such events.” Treatment approaches such as Adaptive Disclosure, Moral Injury Group therapy, and Trauma Informed Guilt Reduction Therapy specifically address the core components of moral injury by focusing on forgiveness, value realignment, and making amends rather than extinguishing fear responses.
The Checkpoint Scenario: A veteran, Sergeant Miller, repeatedly seeks therapy for “anxiety.” Standard PTSD treatments involving exposure therapy require him to recount a checkpoint incident where a civilian vehicle was engaged. However, his physiological response doesn’t spike from fear of dying; it spikes from the shame of the resulting casualties. Treating him for fear fails because the root is a violation of his moral code—he needs therapy focused on forgiveness and atonement, not safety.

Who Are You Without the Uniform?
Leaving military service creates an existential void. Veterans lose their tribe and their mission simultaneously. This loss of identity often presents with symptoms identical to depression, but antidepressants won’t address the underlying issue. The condition requires a reconstruction of the self rather than pharmaceutical intervention. Finding a new purpose to replace the one left behind becomes essential for psychological recovery and social reintegration.
Biology vs. Psychology: The Brain Injury Overlap
Modern veteran mental health support systems are finally examining the physical brain, not just the mind. The overlap between Traumatic Brain Injury (TBI) symptoms and mental health struggles is substantial, and misdiagnosis is rampant. If physical damage to the brain isn’t addressed, talk therapy will reach a therapeutic ceiling. The VA and private healthcare systems are increasingly conducting comprehensive evaluations that include neurological assessments alongside psychological screenings.
Your Body is on Fire (And So is Your Brain)
Chronic stress creates systemic inflammation that affects neurotransmitter function. New protocols involve checking C-reactive protein levels and other inflammatory markers. Treating the body’s inflammatory response often acts as a proxy for treating the mind. Addressing physiological swelling before addressing cognitive distortions can significantly improve treatment outcomes. Veterans looking for actionable ways to reduce inflammation and calm the nervous system can explore resources on managing PTSD for veterans with practical tips for a healthier mind and body.
Fixing Your Broken Sleep Architecture
Trauma physically changes sleep patterns, specifically destroying REM density. Fixing sleep is a foundational step in mental health recovery. Processing trauma is not possible when the brain is exhausted. Treatment is moving toward correcting sleep architecture using Cognitive Behavioral Therapy for Insomnia (CBT-i) or non-habit-forming medications before engaging in heavy emotional processing work. Sleep apnea, which causes micro-waking throughout the night, prevents REM sleep and causes irritability and cognitive decline that can be mistaken for primary psychiatric conditions.
Testosterone Checks Before Treating Depression
Living in “fight or flight” mode depletes testosterone and disrupts cortisol regulation. Every veteran experiencing treatment-resistant depression should undergo a full endocrine panel. Low testosterone presents almost identically to treatment-resistant depression. The condition might require hormone replacement therapy rather than antidepressants.
Checklist: The “Is It Biological?” Pre-Screen
Before accepting a purely psychiatric diagnosis, the VA may review these physical factors:
- Testosterone Levels: (Total and Free Testosterone) Low T mimics depression (lethargy, brain fog, low mood)
- Thyroid Panel: (TSH, T3, T4) Hyperthyroidism can present as anxiety; Hypothyroidism presents as depression
- Vitamin Deficiencies: (Vitamin D, B12, Magnesium) Common in veterans and crucial for mood regulation
- Sleep Apnea Study: Micro-waking throughout the night prevents REM sleep, causing irritability and cognitive decline
- Inflammatory Markers: (C-Reactive Protein) High inflammation is linked to treatment-resistant depression

The Male-Centric Model is Failing Women Veterans
The military demographic is changing, but the care model remains stuck in the past. The “one-size-fits-all” approach doesn’t work for women veterans. They face unique stressors regarding how their service is perceived and deal with different prevalence rates of specific trauma types.
Betrayal from Within the Ranks
Military Sexual Trauma (MST) is fundamentally different from combat trauma. The threat came from inside the unit, not the enemy. The therapeutic approach must prioritize safety and trust-building within the medical environment above all else. Healing from betrayal cannot occur in an environment that feels unsafe or dismissive. Treatment protocols for MST emphasize establishing a therapeutic alliance before processing traumatic memories.
Alternatives to Pills and Talk Therapy
The standard “talk therapy and pills” model is being replaced by physiological and technological interventions. Trauma lives in the body, and accessing the subconscious often requires altered states of consciousness or direct nerve stimulation. Veterans can research clinical trials and ask primary care providers about interventional psychiatry. States are beginning to recognize the need for immediate, non-traditional access; Uwill, the nation’s leading mental health and wellness platform, was awarded and is rolling out a program which provides immediate, confidential veteran mental health support 24/7/365 for Alabama’s veterans.
Hacking the Nervous System Directly
Some treatments bypass the thinking brain entirely to calm the nervous system. These are vital for veterans who find talk therapy ineffective or re-traumatizing. Physiological interventions flip the switch from “danger” to “safety” without requiring verbal processing.
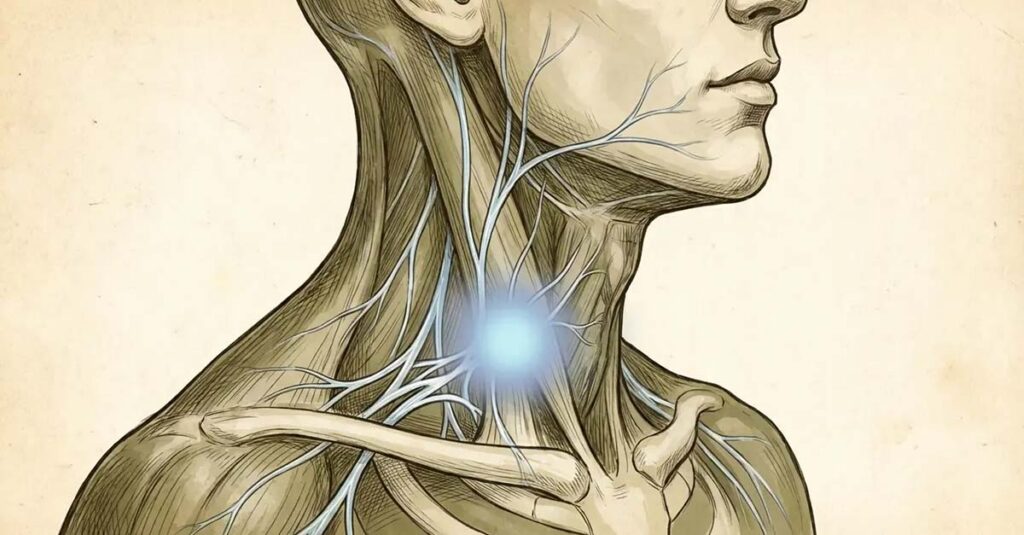
The Stellate Ganglion Block Reboot
SGB involves injecting a local anesthetic into a nerve bundle in the neck. It functions as a “reboot” for the sympathetic nervous system and often provides immediate relief from hyperarousal and anxiety. The stellate ganglion is a cluster of nerve cell bodies located between the C6 and C7 vertebrae, and injection of local anesthetic to this cluster inhibits sympathetic nerve impulses to the head, neck, and upper extremities. This biological reset allows other therapies to take hold. Many veterans report a significant reduction in PTSD symptoms within hours to days after the procedure.
The “Reboot” Effect: Consider a veteran who has been in a state of hypervigilance for 10 years—scanning every rooftop and unable to sit with their back to a door. After receiving a Stellate Ganglion Block (SGB) in the morning, they report going out to dinner that same evening and realizing, for the first time in a decade, they didn’t check the exits. The physical “alarm” in the neck was turned off, allowing the mind to finally rest.
Magnetic Stimulation for Treatment-Resistant Depression
Transcranial Magnetic Stimulation (TMS) uses magnetic fields to stimulate nerve cells. It is non-invasive and FDA-cleared. This represents a crucial alternative for veterans who have seen zero results from traditional antidepressants. TMS directly targets areas of the brain associated with mood regulation and has shown efficacy in treatment-resistant cases where multiple medication trials have failed.

The Psychedelic Renaissance in Veteran Care
Substances like MDMA and Psilocybin are moving from taboo to mainstream treatment options. These therapies allow veterans to revisit traumatic memories without the overwhelming fear response. This is becoming a legitimate frontier in VA and private sector care, with multiple clinical trials underway examining efficacy and safety profiles.
Navigating the Legal Gray Areas
Access is currently limited to clinical trials or ketamine clinics. Veterans must navigate this carefully and ensure they are in a safe, therapeutic setting. The difference between recreational use and clinical application is substantial, and proper medical supervision is essential for safety and therapeutic benefit.
Quieting the Fear Center
The science is straightforward: these compounds reduce activity in the amygdala (the fear center) and increase connectivity in the prefrontal cortex. This allows individuals to process memories with detachment and self-compassion. Traumatic memories can be examined without reliving the physiological terror response that typically accompanies recall.
Why the Trip is Only Half the Work
The drug experience is only 50% of the treatment. “Integration” is essential—working with a therapist in the days following the session to metabolize the insights. Without integration, the experience is just a memory, not a therapeutic intervention.
Tech and Tribe: Healing Outside the Clinic
Healing happens in the community, not just the doctor’s office. Technology and community models are moving away from pathologizing veterans. The goal is reintegration, not just symptom management.

Facing Triggers in Virtual Reality
Virtual Reality Exposure Therapy (VRET) immerses individuals in computer-generated environments that replicate triggers. This allows the brain to extinguish the fear response in a controlled way. Veterans can practice handling a crowded market or a convoy without leaving the safety of the clinic.
The Power of Shared Experience
Veterans respond better to other veterans. Certified Peer Support Specialists are trained veterans who use their own recovery stories to provide support. They bridge the gap between the clinical provider and the patient. Reintegrating into a community is essential, which is why mental health support and finding strength in your veteran connections is a core component of healing.

Nature as a Prescription
Structured time in nature decreases cortisol. “Green therapy” or Ecotherapy isn’t just hiking; it’s a prescribed treatment to reduce hypervigilance. Programs that use evidence-based frameworks rather than just recreational activities show measurable improvements in symptoms.
The Paperwork War: Securing the Benefits You Earned
Accessing advanced treatments hinges on financial stability and VA healthcare access. The VA claims process is a source of mental strain itself. Mental health conditions are invisible, making documentation the single most critical factor in securing support. Veterans cannot rely solely on VA treatment records. Veterans experience elevated rates of suicide compared with the general population, which highlights the importance of access to care and appropriate mental health support.

Proving the Invisible Wounds
Mental health claims require substantial evidence to prove severity and service connection. Unlike a physical injury, subjective conditions lead to denials without precise documentation. Proving the origin of the issue is difficult if help was avoided while active due to stigma. One of the most effective tools for establishing this proof is the “Statement in Support of Claim”; veterans can learn more about VA Form 21-0781 and the statement that supports mental health claims like PTSD to strengthen their case.
Connecting the Dots for the VA
An independent medical opinion connects a current diagnosis to a specific in-service event. A provider must review records and explicitly state the condition is “at least as likely as not” caused by service. This documentation is often the missing link in a denied claim.
Template: Key Elements of an Independent Medical Opinion
- Provider Credentials: “I am a Board Certified Psychologist with X years of experience…”
- Records Reviewed: “I have reviewed the veteran’s service medical records, specifically pages XX-XX…”
- The Rationale: “The veteran’s current condition is consistent with the in-service event described as…”
- What Clinicians Typically Include in a Medical Opinion: Clinicians typically describe whether a condition is medically related to service based on their professional judgment and review of records.”
Overcoming the Lack of Service Records
Proving the origin of mental health issues is challenging without medical records from time in service. “Buddy statements” and performance evaluations serve as proxy evidence for behavioral changes that occurred during service.
Cracking the VA Rating Code
Understanding how the VA rates mental health is essential. The difference between a 30% and a 70% rating comes down to specific keywords regarding social and occupational impairment. If those words aren’t in the record, the rating won’t reflect the true severity.
| Rating | Level of Impairment | Key Symptoms/Criteria |
| 0% | Formal Diagnosis, No Impairment | Symptoms are controlled by medication; no impact on work/social life |
| 30% | Mild Social/Occupational Impairment | Occasional decrease in work efficiency; intermittent inability to perform tasks; chronic sleep impairment |
| 50% | Moderate Impairment | Reduced reliability and productivity; panic attacks weekly; impaired memory; flattened affect |
| 70% | Significant Impairment (Most Common High Rating) | Deficiencies in most areas (work/school/family); suicidal ideation; obsessive rituals; near-constant panic; spatial disorientation |
| 100% | Total Occupational and Social Impairment | Gross impairment in thought processes; persistent delusions; inability to perform daily activities; danger to self or others |
Why the DBQ is Your Most Important Document
Disability Benefits Questionnaires (DBQs) are standardized forms used to document medical findings for VA review.. This specific form must be filled out correctly to ensure the VA can accurately evaluate the claim.

Defining Total Occupational and Social Impairment
This level of impairment reflects severe functional limitations that prevent consistent work or social functioning. It indicates an inability to function in a work or social environment. Documentation must provide concrete examples of this impairment, not just a list of symptoms.
Mental Health as a Secondary Effect
Mental health issues often arise secondary to physical pain. Filing for depression caused by chronic back pain is a viable consideration. Many veterans overlook this nuance when documenting their conditions for VA evaluation.
The “Back Pain to Depression” Link: A veteran is rated 40% for a lumbar strain and sciatica. He cannot run, lift his kids, or sleep through the night due to pain. He has no combat trauma, but he experiences depression due to his physical limitations. He can file a claim for “Depression secondary to Service-Connected Back Pain.” If his doctor provides an independent medical opinion linking the chronic pain to his mental state, he can be rated for depression even without a specific in-service mental health event.
Fueling the Fight: Nutrition and Lifestyle
Sustainable recovery requires a “whole health” approach. Diet and lifestyle choices impact mental resilience. Eliminating inflammatory foods and prioritizing gut health serves as a first line of defense against anxiety.
Your Gut is Your Second Brain
The gut microbiome produces the vast majority of the body’s serotonin. The gut-brain axis is well-established in medical literature. Poor diet directly exacerbates PTSD symptoms. A healthy mind cannot exist with an unhealthy gut.

Eating for Mental Resilience
Nutritional Psychiatry uses food and supplements to manage mental health. Treating the gut lining prevents toxins from entering the bloodstream. Omega-3s and probiotics are tools in the mental health recovery toolkit.
Don’t Let Bad Paperwork Block Your Recovery
Fighting for mental health is hard enough without fighting the bureaucracy too. Mental health documentation can sometimes vary depending on how symptoms are described in clinical records. REE Medical coordinates access to independent medical providers who understand the full scope of service-connected conditions. The network of experts specializes in completing DBQs accurately, ensuring the severity of conditions is documented exactly how the VA needs to see it. Whether veterans need an independent medical evaluation or a proper assessment for an increase, REE Medical coordinates the documentation process to support accurate VA evaluation so veterans can access the care they need. The path to benefits can be complicated, but veterans don’t have to navigate it alone; reading the veteran’s guide on navigating the VA disability system with PTSD clarifies how accurate medical evidence makes all the difference.
The Mission Continues
The landscape of veteran mental health support is evolving rapidly. From understanding moral injury to utilizing psychedelic therapies, the options for healing are expanding. But accessing these resources often requires the financial stability that comes with a proper disability rating. Self-advocacy is essential, both in the clinic and in the claims process. REE Medical coordinates independent medical documentation so veterans can focus on the real work of healing.
DISCLOSURE
DISCLAIMER: REE Medical, LLC is not a Veterans Service Organization (VSO) or a law firm and is not affiliated with the U.S. Veterans Administration (“VA”). Results are not guaranteed, and REE Medical, LLC makes no promises. REE Medical’s staff does not provide medical advice or legal advice, and REE Medical is not a law firm. Any information discussed, such as, but not limited to, the likely chance of an increase or service connection, estimated benefit amounts, and potential new ratings, is solely based on past client generalizations and not specific to any one patient. The doctor has the right to reject and/or refuse to complete a Veteran’s Disability Benefit Questionnaire if they feel the Veteran is not being truthful. The Veteran’s Administration is the only agency that can make a determination regarding whether or not a Veteran will receive an increase in their service-connected disabilities or make a decision on whether or not a disability will be considered service-connected. This business is not sponsored by, or affiliated with, the United States Department of Veterans Affairs, any State Department of Military and Veterans Affairs, or any other federally chartered veterans service organization.